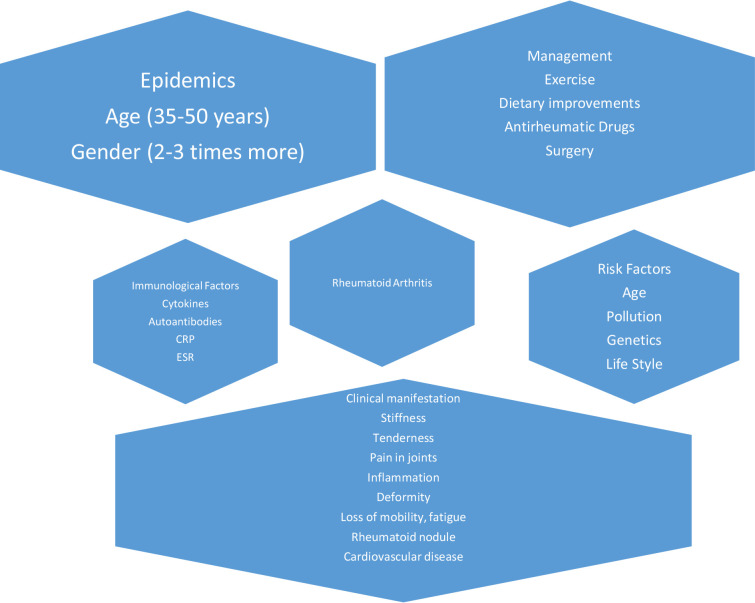
Rheumatoid arthritis (RA) is a long-term disease where the body’s immune system attacks its own joints, but it can also affect other parts of the body. It’s more than joint pain—it can make everyday activities harder. The Mediterranean Journal of Rheumatology says that about 0.5% to 1% of people in the U.S. have rheumatoid arthritis (RA). Around 0.9% of people in India are also affected. This shows that RA is a problem all over the world. If you’ve been diagnosed with RA or are learning about it, this article will explain what it is and give you tips on how to manage its symptoms and live a better life.

What Is Rheumatoid Arthritis?
Rheumatoid arthritis is a long-term autoimmune condition that causes inflammation in the joints. This inflammation leads to pain, swelling, and stiffness in the affected areas. If not treated, the condition can result in damage to the bones and cartilage within the joints. RA causes long-lasting inflammation in the joints, which can damage bones and cartilage. This leads to joint destruction. It usually affects smaller joints, like those in the hands and feet. But, RA can also affect larger joints, such as the knees, shoulders, and elbows.
RA isn’t limited to the joints—it’s a systemic disease, which means it can affect other parts of your body. Many individuals with RA also experience fatigue, fever, weight loss, and general discomfort. Clinical manifestations include morning stiffness, pain in the shoulder, neck, and pelvic girdle, loss of mobility, and the development of rheumatoid nodules. In fact, the symptoms of RA are often worse in the morning, with joint stiffness lasting for an hour or more.
How Does Rheumatoid Arthritis Affect the Body?
In simple terms, rheumatoid arthritis occurs when your immune system, designed to protect you from infections, mistakenly attacks the lining of your joints. This lining, known as the synovium, becomes inflamed and swollen. As a result, the cartilage and bones in the joint may start to break down, which can cause deformities and loss of function.
Research from the Mediterranean Journal of Rheumatology shows that inflammation in RA patients happens because of a cell-based immune response. There are many CD4+ T cells in the affected joints, which suggests that T cells play a harmful role in the disease. B-cells also contribute by producing autoantibodies and creating pro-inflammatory cytokines.
The inflammation from RA can spread beyond the joints. It can affect other parts of the body. Over time, joint damage may get worse. This can lead to permanent changes that limit movement and lower quality of life. Studies show that chronic inflammation in RA patients can also cause heart problems. These issues go beyond regular heart disease risk factors. RA patients have about double the risk of heart disease and may live 3–12 years less.
What Causes Rheumatoid Arthritis?
The exact cause of rheumatoid arthritis (RA) is not fully understood. Experts think it’s caused by a mix of genetic and environmental factors. Studies have found that the HLA-DRB1 gene is a major factor, contributing to 30% to 40% of the genetic risk for RA. Other genes, like TRAF1/C5, IL2RB, and PTPN22, also play important roles. If someone in your family has RA, you’re more likely to develop it. Lifestyle factors, like smoking, infections, and diet, can also affect your chances of getting RA.
Interestingly, RA is more common in women, possibly due to hormonal influences. This may be because of hormonal influences. Studies show that sex hormones like prolactin and oestrogens play a role in RA. Oral contraceptives may help reduce symptoms, especially in patients with anti-CCP antibodies. Many women notice changes in their symptoms during pregnancy. Some feel relief, but others experience flare-ups after childbirth.
Environmental Triggers
Certain environmental factors are linked to the development of rheumatoid arthritis. Increased urbanization, smoking, and exposure to pesticides are significant risk factors. Studies show that people who are exposed to chemicals like organophosphates and chlorimuron ethyl pesticides have higher rates of RA. These factors can trigger RA in people who are already genetically at risk.
Symptoms of Rheumatoid Arthritis
Rheumatoid arthritis can show up in different ways. It usually starts with pain, swelling, and stiffness in the joints, especially in the hands, wrists, and feet. As time goes on, other joints, like the knees, elbows, and ankles, may also be affected.
RA is known for its “flare-ups,” where symptoms worsen for a time before improving again. Common symptoms of RA include:
Common Symptoms of RA
- Fatigue: Many people with RA experience extreme tiredness, even after a full night’s sleep.
- Low-grade fever: A mild fever is often present.
- Loss of appetite: RA can cause a lack of interest in food, leading to weight loss.
- Rheumatoid nodules: Small lumps that can form under the skin, usually near the elbows or hands.
- Joint pain and stiffness: This is the most noticeable symptom of RA, often worse in the morning and lasting for several hours.
Extra Symptoms and Complications
In some cases, RA can affect other organs, like the eyes, lungs, and heart. This can lead to more complications. Lung problems, such as pleural effusion and obstructive lung disorders, are common and cause 10–20% of deaths in RA patients. Eye issues, like episcleritis and scleromalacia, occur in about 27% of patients.
How Is Rheumatoid Arthritis Diagnosed?
Rheumatoid arthritis is diagnosed with physical exams, blood tests, and imaging. Doctors check for joint tenderness, warmth, or swelling. Blood tests can show signs of inflammation or specific proteins linked to RA, like rheumatoid factor and anti-CCP antibodies.
Advanced Diagnostic Criteria and Tools
The American College of Rheumatology (ACR) 2010 criteria, developed by the European League Against Rheumatism (EULAR), are now used for diagnosis. These criteria are more sensitive in detecting early RA. The Disease Activity Score 28 (DAS 28) is often used to measure disease activity. It counts 28 tender and swollen joints. Imaging tests like X-rays and ultrasounds can show joint damage and track disease progression. Advanced imaging techniques, such as Doppler ultrasound and MRI, provide a detailed view of joint damage and are linked to more severe disease.
Treatment Options for Rheumatoid Arthritis
There is no cure for rheumatoid arthritis, but there are treatments that can help. These treatments manage symptoms, slow down the disease, and improve quality of life. The goal is to reduce pain, prevent joint damage, and make movement easier and more comfortable.
Medications
There are various medications available to treat RA. Some focus on reducing inflammation, while others slow the disease’s progression.
- Pain relievers: Medications like ibuprofen and naproxen can provide short-term relief from pain and inflammation.
- Steroids: Prednisone is commonly used to reduce inflammation quickly, particularly during flare-ups.
- Disease-modifying antirheumatic drugs (DMARDs): These medications help slow RA and prevent more joint damage. Methotrexate (MTX) is often the first choice.
- Biologics: Biologics like etanercept and adalimumab target parts of the immune system to stop inflammation.
- New oral medications: Medications like tofacitinib block enzymes that cause inflammation.
Lifestyle Changes
Making lifestyle changes can help reduce the severity of rheumatoid arthritis and improve your quality of life. Regular exercise, especially low-impact activities like swimming, walking, or cycling, is important. These activities help keep your joints flexible and strengthen the muscles around them. Studies show that personalized exercise programs can improve fitness and reduce RA symptoms. They also lower the risk of heart disease.
A balanced, anti-inflammatory diet with fruits, vegetables, and omega-3 fatty acids can help reduce inflammation. Many people with RA find that some foods make symptoms better or worse. It’s important to watch how your body reacts to different foods.
Surgery
In severe cases, surgery may be needed. Joint replacement surgery, especially in the hips, knees, and shoulders, can help restore movement and reduce pain.
Managing Life with Rheumatoid Arthritis
Living with rheumatoid arthritis can be tough, but it’s important to remember that you don’t have to face it alone. Many people with RA lead full, active lives with the right treatment and support. Working with your doctor to create a tailored treatment plan is crucial. Additionally, there are resources like occupational therapy, physical therapy, and support groups that can be incredibly helpful.
Rehabilitation and Support
Rehabilitation is important for managing RA. It helps improve or maintain your quality of life by restoring normal functions and reducing problems. Occupational therapists help patients with daily activities, making them more independent and able to work. Assistive devices, like braces or special tools, can make tasks easier. Don’t be afraid to ask for help when you need it. Focus on self-care and listen to your body.
Final Thoughts on Rheumatoid Arthritis
Rheumatoid arthritis can make life harder, but you can manage the symptoms. With the right treatment, including medications, physical therapy, lifestyle changes, and emotional support, you can take control of your health. It’s possible to live a fulfilling life despite the challenges.
Expert Insights and Future Directions
Current research highlights the importance of a complete treatment plan. This plan includes both medication and lifestyle changes. New biological treatments and personalized medicine are also showing promise. Artificial intelligence is being used to predict the best treatments. These advances give hope for better management of RA.
Recent studies show that combining rehabilitation with medical treatments can help. It improves joint movement and function. It also boosts independence and quality of life for people with RA.
If you’re dealing with rheumatoid arthritis, talk to your healthcare provider about the best treatment options for your needs. Start by making small, positive changes every day to stay active and healthy. Remember, you’re not alone—support is available.
Take Charge of Your Rheumatoid Arthritis Treatment
Dealing with rheumatoid arthritis can be overwhelming. The good news is that treatment options have improved a lot. There are now medications and lifestyle changes that can help manage the condition. Research is also showing how genetics and the environment play a role in RA. Because of this, personalized treatment plans are becoming more common and effective. If you’re having trouble with symptoms, talk to your doctor about treatments that can really help.
Sources: